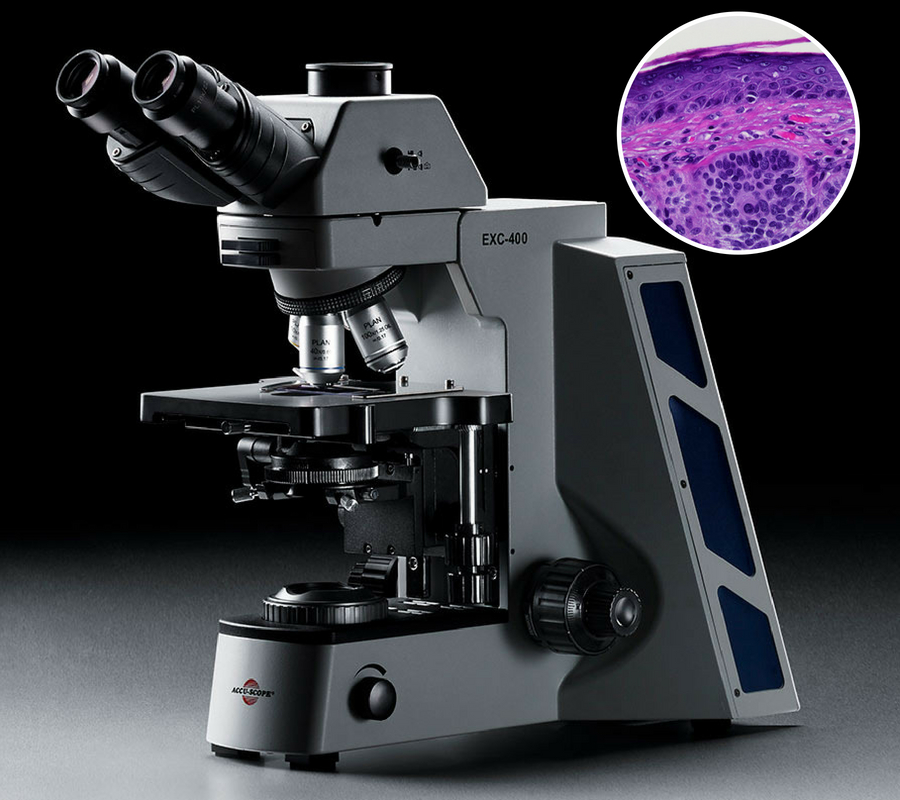
A tiny section of skin, sliced, stained, placed on a glass slide and magnified on a special microscope, may look pretty, but it could reveal skin cancer. Photo by Yasu + Junko; microscope provided by Accu-scope.
Skin lesions don’t come with labels, bells or whistles. Diagnosing skin cancer is way more complicated than you might think. Our two-part article gives you a peek behind the scenes of this little-understood but fascinating area of dermatology.
Part 1 described how a dermatologist performs a skin exam and determines if all or part of a suspicious spot or lesion should be removed and sent to a lab for a biopsy. It also discussed the highly trained medical specialists (dermatopathologists) who analyze the tissue, and why that is so important. Part two reveals what happens to your biopsy tissue sample, step by step, after your dermatologist ships it off to the lab.
Ever wonder what happens to that little piece of skin after it’s removed from your body? The tissue, which has been “fixed” so it doesn’t change or degrade, is transported to the lab in a small jar or bottle. It can stay at room temperature and doesn’t need to be refrigerated. Once at the lab, it is logged in, and the specimen goes through several steps of processing to help the dermatopathologist analyze it under a microscope to determine a diagnosis. See our slide show. (Lab photos courtesy of Yale Department of Dermatology).
A Biopsy Tissue Sample’s Journey